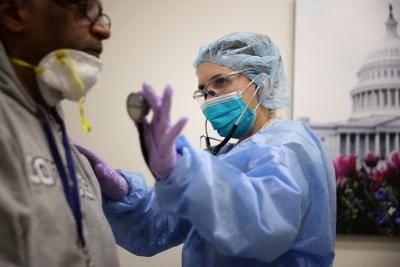
A controversial debate during COVID-19 is the state of readiness within governments and health systems for a pandemic, with lines of the debate drawn on the issues of testing provision, personal protective equipment (PPE), and the speed of decision-making.
President Macron in a speech to the nation admitted French medical workers did not have enough PPE and that mistakes had been made: ‘Were we prepared for this crisis? We have to say that no, we weren’t, but we have to admit our errors … and we will learn from this’.
In reality few governments were fully prepared. In years to come, all will ask: ‘how could we have been better prepared, what did we do wrong, and what can we learn?’. But after every crisis, governments ask these same questions.
Most countries have put in place national risk assessments and established processes and systems to monitor and stress-test crisis-preparedness. So why have some countries been seemingly better prepared?
Comparing different approaches
Some have had more time and been able to watch the spread of the disease and learn from those countries that had it first. Others have taken their own routes, and there will be much to learn from comparing these different approaches in the longer run.
Governments in Asia have been strongly influenced by the experience of the SARS epidemic in 2002-3 and - South Korea in particular - the MERS-CoV outbreak in 2015 which was the largest outside the Middle East. Several carried out preparatory work in terms of risk assessment, preparedness measures and resilience planning for a wide range of threats.
Case Study of Preparedness: South KoreaBy 2007, South Korea had established the Division of Public Health Crisis Response in Korea Centers for Disease Control and Prevention (KCDC) and, in 2016, the KCDC Center for Public Health Emergency Preparedness and Response had established a round-the-clock Emergency Operations Center with rapid response teams. KCDC is responsible for the distribution of antiviral stockpiles to 16 cities and provinces that are required by law to hold and manage antiviral stockpiles. |
And, at the international level, there are frameworks for preparedness for pandemics. The International Health Regulations (IHR) - adopted at the 2005 World Health Assembly and binding on member states - require countries to report certain disease outbreaks and public health events to the World Health Organization (WHO) and ‘prevent, protect against, control and provide a public health response to the international spread of disease in ways that are commensurate with and restricted to public health risks, and which avoid unnecessary interference with international traffic and trade’.
Under IHR, governments committed to a programme of building core capacities including coordination, surveillance, response and preparedness. The UN Sendai Framework for Disaster Risk highlights disaster preparedness for effective response as one of its main purposes and has already incorporated these measures into the Sustainable Development Goals (SDGs) and other Agenda 2030 initiatives. UN Secretary-General António Guterres has said COVID-19 ‘poses a significant threat to the maintenance of international peace and security’ and that ‘a signal of unity and resolve from the Council would count for a lot at this anxious time’.
Case Study of Preparedness: United StatesThe National Institutes of Health (NIH) and the Center for Disease Control (CDC) established PERRC – the Preparedness for Emergency Response Research Centers - as a requirement of the 2006 Pandemic and All-Hazards Preparedness Act, which required research to ‘improve federal, state, local, and tribal public health preparedness and response systems’. The 2006 Act has since been supplanted by the 2019 Pandemic and All-Hazards Preparedness and Advancing Innovation Act. This created the post of Assistant Secretary for Preparedness and Response (ASPR) in the Department for Health and Human Services (HHS) and authorised the development and acquisitions of medical countermeasures and a quadrennial National Health Security Strategy. The 2019 Act also set in place a number of measures including the requirement for the US government to re-evaluate several important metrics of the Public Health Emergency Preparedness cooperative agreement and the Hospital Preparedness Program, and a requirement for a report on the states of preparedness and response in US healthcare facilities. |
This pandemic looks set to continue to be a grave threat to humanity. But there will also be future pandemics – whether another type of coronavirus or a new influenza virus – and our species will be threatened again, we just don’t know when.
Other disasters too will befall us – we already see the impacts of climate change arriving on our doorsteps characterised by increased numbers and intensity of floods, hurricanes, fires, crop failure and other manifestations of a warming, increasingly turbulent atmosphere and we will continue to suffer major volcanic eruptions, earthquakes and tsunamis. All high impact, unknown probability events.
Preparedness for an unknown future is expensive and requires a great deal of effort for events that may not happen within the preparers’ lifetimes. It is hard to imagine now, but people will forget this crisis, and revert to their imagined projections of the future where crises don’t occur, and progress follows progress. But history shows us otherwise.
Preparations for future crises always fall prey to financial cuts and austerity measures in lean times unless there is a mechanism to prevent that. Cost-benefit analyses will understandably tend to prioritise the urgent over the long-term. So governments should put in place legislation – or strengthen existing legislation – now to ensure their countries are as prepared as possible for whatever crisis is coming.
Such a legal requirement would require governments to report back to parliament every year on the state of their national preparations detailing such measures as:
- The exact levels of stocks of essential materials (including medical equipment)
- The ability of hospitals to cope with large influx of patients
- How many drills, exercises and simulations had been organised – and their findings
- What was being done to implement lessons learned & improve preparedness
In addition, further actions should be taken:
- Parliamentary committees such as the UK Joint Committee on the National Security Strategy should scrutinise the government’s readiness for the potential threats outlined in the National Risk register for Civil Emergencies in-depth on an annual basis.
- Parliamentarians, including ministers, with responsibility for national security and resilience should participate in drills, table-top exercises and simulations to see for themselves the problems inherent with dealing with crises.
- All governments should have a minister (or equivalent) with the sole responsibility for national crisis preparedness and resilience. The Minister would be empowered to liaise internationally and coordinate local responses such as local resilience groups.
- There should be ring-fenced budget lines in annual budgets specifically for preparedness and resilience measures, annually reported on and assessed by parliaments as part of the due diligence process.
And at the international level:
- The UN Security Council should establish a Crisis Preparedness Committee to bolster the ability of United Nations Member States to respond to international crisis such as pandemics, within their borders and across regions. The Committee would function in a similar fashion as the Counter Terrorism Committee that was established following the 9/11 terrorist attacks in the United States.
- States should present reports on their level of preparedness to the UN Security Council. The Crisis Preparedness Committee could establish a group of experts who would conduct expert assessments of each member state’s risks and preparedness and facilitate technical assistance as required.
- Regional bodies such as the OSCE, ASEAN and ARF, the AU, the OAS, the PIF etc could also request national reports on crisis preparedness for discussion and cooperation at the regional level.
COVID-19 has been referred to as the 9/11 of crisis preparedness and response. Just as that shocking terrorist attack shifted the world and created a series of measures to address terrorism, we now recognise our security frameworks need far more emphasis on being prepared and being resilient. Whatever has been done in the past, it is clear that was nowhere near enough and that has to change.
Case Study of Preparedness: The UKThe National Risk Register was first published in 2008 as part of the undertakings laid out in the National Security Strategy (the UK also published the Biological Security Strategy in July 2018). Now entitled the National Risk Register for Civil Emergencies it has been updated regularly to analyse the risks of major emergencies that could affect the UK in the next five years and provide resilience advice and guidance. The latest edition - produced in 2017 when the UK had a Minister for Government Resilience and Efficiency - placed the risk of a pandemic influenza in the ‘highly likely and most severe’ category. It stood out from all the other identified risks, whereas an emerging disease (such as COVID-19) was identified as ‘highly likely but with moderate impact’. However, much preparatory work for an influenza pandemic is the same as for COVID-19, particularly in prepositioning large stocks of PPE, readiness within large hospitals, and the creation of new hospitals and facilities. One key issue is that the 2017 NHS Operating Framework for Managing the Response to Pandemic Influenza was dependent on pre-positioned ’just in case’ stockpiles of PPE. But as it became clear the PPE stocks were not adequate for the pandemic, it was reported that recommendations about the stockpile by NERVTAG (the New and Emerging Respiratory Virus Threats Advisory Group which advises the government on the threat posed by new and emerging respiratory viruses) had been subjected to an ‘economic assessment’ and decisions reversed on, for example, eye protection. The UK chief medical officer Dame Sally Davies, when speaking at the World Health Organization about Operation Cygnus – a 2016 three-day exercise on a flu pandemic in the UK – reportedly said the UK was not ready for a severe flu attack and ‘a lot of things need improving’. Aware of the significance of the situation, the UK Parliamentary Joint Committee on the National Security Strategy launched an inquiry in 2019 on ‘Biosecurity and human health: preparing for emerging infectious diseases and bioweapons’ which intended to coordinate a cross-government approach to biosecurity threats. But the inquiry had to postpone its oral hearings scheduled for late October 2019 and, because of the general election in December 2019, the committee was obliged to close the inquiry. |